Do you know the warning signs of Pelvic Congestion Syndrome (PCS)? (Also known as ovarian vein reflux?) While pelvic pain, incontinence and uterine fibroids often go hand in hand, these are also red flags for other serious conditions. One such problem is PCS, a medical problem that is triggered by internal varicose veins in your lower abdomen and pelvis. 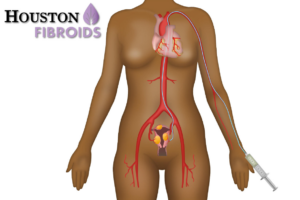
Typically, these veins are in your ovaries. They form with vein reflux (when blood flows backward in your veins). The kind of pelvic pain connected with PCS is more of a chronic ache; some women describe the sensation of someone tugging or pulling in their pelvis.
PCS is a long-term condition, meaning symptoms will stick around. In fact, the diagnosis is usually made after 6 months of chronic pelvic pain without signs of an inflammatory condition. Yet, with this problem, the pain can be made worse when you first stand up or first sit down. Lying down, on the other hand, can provide relief from the pain of PCS.
In addition to pain in your pelvis and lower back, PCS can trigger an irritable bowel and/or bladder and painful sex. PCS may also cause visible varicose veins to appear in or around your vulva, vagina, perineum and anus. Additionally, with this condition, your pelvis can feel an uncomfortable sensation of fullness.
PCS is fairly common, and is the underlying cause of chronic pelvic pain for between 13 and 40% of women, according to the British Society of Interventional Radiology. Yet it is often misdiagnosed as Polycisystic Ovarian Syndrome (PCOS), Premenstrual Dysphoric Disorder (PMDD) or endometriosis, likely because the symptoms mimic other conditions, and the root cause of the problem is buried deep within your body. That was certainly the case for Johnelle Mercer, a 19-year old woman from Las Vegas who spent years suffering before finally getting diagnosed.
From the time of her very first period, Mercer experienced terrible pelvic pain. Her periods were very heavy, and she lived with breakthrough bleeding between periods. But every time she discussed her symptoms with doctors, they told her she was just stuck with bad periods.
Sick of being ignored and dismissed, this brave young woman kept advocating to get a diagnosis that would offer pain relief. Finally, at the age of 19, she received that diagnosis: PCS. We're celebrating her as our Woman Crush of the Week for refusing to be ignored. (And for sharing her PCS diagnosis experience with this viral Tik Tok video.)
Also, we're helping you understand more about this hard-to-diagnose source of pelvic pain. Because we want you to find relief sooner than Johnelle did. And, with that in mind, here’s what you need to know about PCS in order to receive the proper diagnosis and treatment:
When too much blood builds up in your pelvic, you develop this painful PCS condition. And internal varicose veins are often at fault. Individuals with PCS will experience a dull, aching pelvis period over an extended period of time. Women are more likely to develop PCS than men, but both genders can be affected.
When men are affected by PCS, the condition is easier to diagnose and treat, because two of men’s four pelvic veins are visible on the outside of their bodies. Because all of women’s pelvic veins are invisible on the surface of their bodies, PCS can be harder to spot for women. Most women with PCS have previously been pregnant, but even women who’ve never had a pregnancy can develop the condition.
Typically, we think of PCS as a problem for premenopausal women. Recently, studies suggest that menopause doesn't always offer relief from PCS. In fact, it turns out that some women first develop symptoms after menopause. Clearly, we need to learn more about the causes of this condition.

As we already mentioned, PCS develops because of varicose pelvic veins. Varicose veins in the pelvis begin to develop when their valves fail, causing blood that should be pushed out of the pelvis to stick around in the area instead of traveling back to the heart. When this happens, the veins become dilated and put pressure on sensitive areas of the pelvis and on the pelvic floor muscles (the ones you exercise when doing your kegels.)
Again, women who've had at least one pregnancy are also more likely to develop this condition. And that's likely because carrying a baby brings more blood flow to the area.
Still, we aren't clear why your valves would fail. Sometimes, the cause seems to be late-pregnancy injury. In other cases, excess estrogen may be the cause, since the hormone can widen your blood vessels. PCS may also be a secondary symptom for people with May-Thurner syndromes. Regardless of the cause, the condition presents with uniform symptoms.
PCS usually causes women to experience pain deep in their pelvis or uterus; the pain is usually dull or aching rather than sharp or intense. PCS pain gets worse all day, especially if you exercise.
While PCS pain is typically dull, changes in posture or heavy lifting can cause women to experience sharp pains in their abdominal area. With PCS, sex and periods can also become more painful.
Some women with PCS also have bladder symptoms that include a frequent need to pee, frequent nighttime trips to the bathroom and even incontinence. Many women will also develop vaginal or vulvar varicose veins. On diagnostic imaging, we'll also notice an increase in the volume of your pelvic veins. And for men and women, PCS can also cause or worsen conditions such as Irritable Bowel Syndrome (IBS), or lead to chronic fatigue and back pain.
We typically diagnose PCS with an ultrasound scan. Then, your Houston interventional radiologists treat PCS easily, with Pelvic Vein Embolisation (PVE). (This is a procedure that's similar to Uterine Fibroid Embolization, or UFE.) Recently, the Society of Vascular Surgeons endorsed this treatment option for resolving PCS.
We use a local anesthetic for this x-ray technique. Guided by ultrasound, we'll insert a catheter (thin tube) in your vein, pushing into the problematic pelvic vein. Once there, we deposit embolizing material to permanently block off the vein or veins causing your PCS symptoms. After, blood can't build up in the area. Your vein will shrink and symptoms should resolve quickly.
With proper care and a minimally invasive procedure, we can quickly treat and resolve PCS. Our highly trained vein specialists can easily spot your PCS symptoms and recommend a treatment plan. If you’re experiencing dull, aching pelvic pain, you should schedule a consultation right away. We can even meet remotely, with a Telemedicine appointment, if that's easier for your current schedule. Remember, you don’t have to live with chronic pelvis pain—you just need to receive the proper diagnosis and treatment plan!
Sources: www.Cedars-Sinai.Org

Scheduling
Please contact our dedicated specialists to schedule a consultation today.
2024 Houston Fibroids. All rights reserved. Website Design by Healthcare Success